The role of diagnostic imaging in sleep research.
By Regina Patrick, RPSGT
X-ray imaging technology first allowed sleep researchers to noninvasively view discrete anatomical differences such as a narrowed oropharynx in OSA patients that could result in abnormal sleep. However, x-ray imaging has limitations. Images can give only a two-dimensional (2D) shadowy silhouette-like view of organs within the body; distinct features of individual organs are not apparent; some organs can be seen only if the person is imaged from a certain position and even this may give limited information; and an image cannot reveal neural or metabolic activity occurring within an organ. More recently developed imaging technologies are counteracting these limitations. Computed tomography (CT), magnetic resonance imaging (MRI), positron emission tomography (PET), single photon emission computed tomography (SPECT), magnetoencephalography (MEG), and low resonance electromagnetic tomography (LORETA) are imaging technologies that now allow scientists to have a three-dimensional (3D) view of organs within the body, to see individual organs distinctly, and to view an organ’s metabolic activity. These expanded capabilities are now enhancing diagnosis, treatment, and sleep medicine research.
COMPUTED TOMOGRAPHY
| Subscribe to Sleep Report for the latest research findings. |
CT is a specialized x-ray imaging technique that allows the body to be viewed in thin slices. In a CT study, a person lies flat on a platform, which is slowly inserted into the cylindrical opening in the center of the CT scanner. The scanner contains a ring that revolves around the patient; the ring consists of an x-ray tube and an x-ray detector array that are positioned opposite to each other. The tube emits x-rays in a thin beam across the area being studied, while the detector array records the emission of x-rays passing through the body. The ring then rotates a few degrees, and another x-ray beam is emitted across the same area. This continues until the ring has made a full revolution around the body. As the ring revolves around the patient, the detector array sends information to a computer for image reconstruction. The resulting image shows a 2D axial slice of the area being imaged as if looking along the body’s long axis running from the top of the head toward the feet. The platform incrementally moves up as each slice is imaged. Because the body can be viewed in axial slices, a physician can more easily view individual organs, which would normally be hidden behind other organs in an x-ray image.
Today in sleep medicine, CT plays a role in diagnosis and treatment in OSA by clearly showing which specific area in the oropharynx—the soft palate, epiglottis, palatine tonsils, or base of the tongue—is the source of airway blockage during apnea episodes. Knowing this subtle difference helps physicians decide the best approach to OSA surgery. This, in turn, can enhance one’s response to OSA surgeries, such as the uvulopalatopharyngoplasty (UPPP, which widens the upper airway by removing excess fatty tissue, the tonsils, and uvula); lateral pharyngoplasty (shortens certain pharyngeal muscles to prevent the lateral inward collapse of the upper airway); palatal stiffening (slender implants are inserted into the soft palate to stiffen it and prevent its collapse into the upper airway); or tongue reduction (it shrinks discrete portions of the tongue base to prevent its blocking the airway).
MAGNETIC RESONANCE IMAGING
MRI utilizes a quality of the atom called resonance. When exposed to a strong external magnetic field, the axis of an atom’s nucleus aligns with that of the magnetic field. During alignment, the atom absorbs energy. If the axial alignment is then disrupted by an electromagnetic force, the atom emits radiofrequency waves. The phenomenon of absorbing and emitting energy in response to magnetic forces is called magnetic resonance. Each element has a characteristic magnetic resonance and can undergo magnetic resonance within body tissues. As a consequence, each type of tissue has a different magnetic resonance.1 This difference allows MRI technology to create 3D, distinct anatomical images.

 |
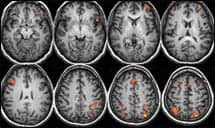
| Brain activation in an SDB patient while performing a working memory task. The images show activations mainly in the prefrontal, frontal precentral, and parietal regions. |
A variation on MRI is functional MRI (fMRI). It differs from conventional MRI in that it creates images by utilizing the difference in magnetic resonance between two molecules found in blood: deoxyhemoglobin and oxyhemoglobin. Deoxyhemoglobin (a hemoglobin molecule that has lost oxygen atoms) has a smaller magnetic resonance than oxyhemoglobin (a hemoglobin molecule that contains oxygen molecules). An fMRI scanner creates images much more quickly than conventional MRI since the amounts of deoxyhemoglobin and oxyhemoglobin are always fluctuating in response to a tissue’s changing oxygen needs. This feature makes fMRI ideal for viewing neural activation in the brain as reflected by blood flow changes.
Sleep researchers have recently begun using fMRI to learn how areas in the brain involved in cognitive functions are impacted by sleep deprivation. For example, researchers at the Stanford Sleep Clinic and Center for Human Sleep Research* are currently using fMRI to study the effect of long-term continuous positive airway pressure (CPAP) treatment on various aspects of memory. Dr Olga Prilipko, one of the investigators of the Stanford study, explains, “Our study is to view how brain activation changes before and after CPAP treatment. We want to know: Does CPAP change how the brain is activated in response to the memory task?” Of particular interest is learning how CPAP treatment affects activation of brain areas involved in memory encoding and working memory, and determining if any change in these cognitive functions correlates to brain activation changes after CPAP treatment. A similar fMRI study by Thomas and coworkers,2 which investigated the impact of OSA and OSA treatment on working memory, found that OSA subjects had decreased activation in the prefrontal and parietal regions when performing memory tasks before bilevel or continuous positive airway pressure treatment. The parietal region recovered some activation after treatment, but the prefrontal region did not. From this, Thomas et al concluded that cognitive dysfunctions in OSA sufferers may not be a consequence of sleep deprivation resulting from the disorder but may be a consequence of an underlying impairment of activation of certain areas involved in cognition.
fMRI also has been used to investigate brain activation in other sleep disorders. For example, research studies have found that the technology may be useful in determining vulnerability to sleep deprivation3, in understanding residual sleepiness in treated narcoleptics4; and in understanding the impaired neural activation resulting in Cheyne-Stokes respiration.5
POSITRON EMISSION TOMOGRAPHY
PET forms images by utilizing radioactivity. The unstable nucleus of an isotope readily disintegrates and may emit in the process positrons, photons, gamma rays, or x-rays.
A PET study involves two steps. First, an isotope is incorporated into a molecule such as glucose or water. The radioactive substance is then injected into a patient. The isotope gives off positrons as the radioactive substance spreads throughout body tissues. When a positron strikes an electron within body tissues, the encounter creates two gamma rays. Areas where high metabolism is occurring will use more of the radioactive substance and therefore will have higher gamma radiation. In the second step of a PET study, a person is slowly inserted on a platform through the cylindrical opening in the center of the PET scanner. The scanner contains a ring that is an array of detectors that record gamma radiation emitted by the person. The detector array sends the information to a computer, which generates a 2D axial slice of the area being studied that shows areas of high gamma radiation (ie, “hot spot,” indicating a high rate of metabolism) and low gamma radiation (indicating less metabolic activity). The image may be color-coded with red typically representing areas of high metabolic activity; green, neutral activity; and blue, low activity. Because a PET image provides a metabolic rather than anatomic depiction of the body, a CT or MRI scan is sometimes done simultaneously with a PET scan, and the two images are overlaid to give a more anatomic rendering of metabolic activity.
PET is used in sleep medicine research to view neural activity in the brain. However, because of the time involved in its two-step process, PET can not record quickly occurring neural activity as can fMRI. PET is used instead to view longer-lasting activity in the brain such as regional activity throughout a sleep period,6 brain activation in restless leg syndrome and other movement disorders during sleep,7,8 and brain activation after sleep deprivation.9
SINGLE PHOTON EMISSION COMPUTED TOMOGRAPHY
SPECT also utilizes radioactivity. The isotope used in SPECT releases on disintegration a single high-energy particle—a photon—which has no weight and no electrical charge. SPECT is sometimes used instead of PET since the decay time of the isotope used in SPECT is longer than that used in PET, the isotope is easier to handle, and SPECT equipment is more readily available.
A SPECT study, like a PET study, is a two-step process in which the radioactive substance is injected in a person who is then placed within the SPECT scanner. The scanner contains a photon detector, which revolves around the person as body tissues radiate photons. The detector moves incrementally by a few degrees to collect data until it has made a full revolution around the person’s body. One full revolution results in an image of one axial slice of the area being studied. The photon detector sends the information to a computer for image reconstruction. The computer creates a metabolic rendering using different colors to denote different levels of activity. For example, silver may represent highest activity; red, normal; yellow, decreased activity; and blue, lowest activity.
In sleep medicine research, SPECT has been used to examine brain activation in narcoleptics,10 investigate impaired sleep in neurological disorders,11 and investigate the effect of sleep deprivation in depressed people.12 Currently, some studies verify what is already known—for example, decreased activation of the hypocretin system in narcoleptics—while other studies reveal new aspects of sleep disorders, including findings that depressed people who have increased activation of some limbic structures respond more readily to sleep deprivation with improved mood.
MAGNETOENCEPHALOGRAPHY
MEG utilizes the magnetic qualities associated with electrical activity. Electrical activity traveling in one direction produces a magnetic field that surrounds the axis of the current. In the brain, a magnetic field can exist around a neuron since its electrical activity flows in one direction from the dendrite, through the cell body, and finally through the axon.
In an MEG study, a person wears a special helmet, which contains an array of superconducting quantum interference devices (SQUIDs, a type of magnetometer) that collect magnetic signals from various points around the head. The SQUIDs relay the information to a computer, which produces an image that shows the magnetic field pattern of the cortex. An MEG image uses colorization to represent activity of the electromagnetic fields, typically using red to represent areas of high electromagnetic activity (increased neural activity) and blue to represent low electromagnetic activity (decreased neural activity). An MEG magnetic field pattern can be overlaid with images produced by fMRI to give a 3D anatomical rendering of electromagnetic activity of the brain.
Sleep researchers have used MEG to investigate various aspects of sleep such as waves in the subdelta range (0.1–0.9 Hz),13 pain perception during sleep,14,15 and changes in electromagnetic activity with mental tasks.16 Results of these studies are beginning to help scientists understand the connection between the voluntary and autonomic functions; how the brain processes pain; and how the brain is activated by different kinds of tasks.
LOW RESONANCE ELECTROMAGNETIC TOMOGRAPHY
LORETA produces tomographic images of electromagnetic activity of the brain. Whereas MEG looks at electromagnetic activity occurring at the cortex of the brain, LORETA uses cortical electromagnetic activity to estimate where within the brain the activity is originating.
In an MEG study, a person wears a special cap that contains sensors for collecting electromagnetic signals. Each sensor relays its information to a computer, which uses the information to create a source map of electromagnetic activity. Since the source of electromagnetic activity cannot be exactly pinpointed but only approximated to a particular area, the resulting map is said to have a low resolution. An MRI scan can be used in conjunction with a LORETA source map to give 3D anatomic rendering of the electromagnetic activity of the brain.
LORETA is being used in sleep medicine research to study the phenomenon of cyclic alternating pattern17 (CAP, transient arousals that are interspersed in the tonic activity of non-rapid eye movement sleep), electromagnetic activation differences between insomniac and noninsomniac subjects,18 the effect of drug therapy on vigilance in post-menopausal women,19,20 and the effect of drug treatment in narcoleptics21; and to analyze various aspects of sleep stages such as spindling.22 Such studies are revealing differences in response to medication and verifying brain activation changes that occur in sleep disorders such as insomnia and narcolepsy.
Future sleep research studies using CT, MRI, PET, SPECT, MEG, and LORETA technologies may soon overturn long-held ideas about what constitutes “normal” sleep. Currently, these imaging technologies are giving sleep researchers new avenues to investigate concerning sleep.
Regina Patrick, RPSGT, is a contributing writer to Sleep Review.
REFERENCES
- Damadian R, Zaner K, Hor D, DiMaio T. Human tumors detected by nuclear magnetic resonance. Proc Natl Acad Sci USA. 1974;71:1471–1473.
- Thomas RJ, Rosen BR, Stern CE, et al. Functional imaging of working memory in obstructive sleep-disordered breathing. J Applied Physiol. 2005;98:2226–2234.
- Lim J, Choo WC, Chee MW. Reproducibility of changes in behaviour and fMRI activation associated with sleep deprivation in a working memory task. Sleep. 2007;30:61–70.
- Thomas RJ. Fatigue in the executive cortical network demonstrated in narcoleptics using functional magnetic resonance imaging—a preliminary study. Sleep Med. 2005;6:399–406.
- Henderson LA, Macey KE, Macey PM, Woo MA, Yan-Go FL, Harper RM. Regional brain response patterns to Cheyne-Stokes breathing. Respir Physiol Neurobiol. 2006;150:87–93.
- Braun AR, Balkin TJ, Wesenten NJ, et al. Regional cerebral blood flow throughout the sleep-wake cycle. An H2(15)O PET study. Brain. 1997;120:1173–1197.
- Cervenka S, Palhagen SE, Comley RA, et al. Support for dopaminergic hypoactivity in restless legs syndrome: a PET study on D2-receptor binding. Brain. 2006;129(Pt 8):2017–2028.
- Hilker R, Razai N, Ghaemi M, et al. [18F]fluorodopa uptake in the upper brainstem measured with positron emission tomography correlates with decreased REM sleep duration in early Parkinson’s disease. Clin Neurol Neurosurg. 2003;105:262–269.
- Gillin JC, Buchsbaum M, Wu J, Clark C, Bunney W Jr. Sleep deprivation as a model experimental antidepressant treatment: findings from functional brain imaging. Depress Anxiety. 2001;14:37–49.
- Joo EY, Hong SB, Tae WS, et al. Cerebral perfusion abnormality in narcolepsy with cataplexy. Neuroimage. 2005;28:410–416.
- Matsui H, Nishinaka K, Oda M, et al. Excessive daytime sleepiness in Parkinson disease: a SPECT study. Sleep. 2006;29:917–920.
- Ebert D, Feistel H, Barocka A, Kaschka W. Increased limbic blood flow and total sleep deprivation in major depression with melancholia. Psychiatry Res. 1994;55:101–109.
- Rodin E, Funke M. Cerebral electromagnetic activity in the subdelta range. J Clin Neurophysiol. 2006;23:238–244.
- Kakigi R, Naka D, Okusa T, et al. Sensory perception during sleep in humans: a magnetoencephalographic study. Sleep Med. 2003;4:493–507.
- Wang X, Inui K, Qiu Y, Kakigi R. Cortical responses to noxious stimuli during sleep.Neuroscience. 2004;128:177–186.
- Fell J, Roschke J, Grozinger M, et al. Alterations of continuous MEG measures during mental activities. Neuropsychobiology. 2000;42:99–106.
- Ferri R, Bruni O, Miano S, Terzano MG. Topographic mapping of the spectral components of the cyclic alternating pattern (CAP). Sleep Med. 2005;6:29–36.
- Szelenberger W, Niemcewicz S. Event-related current density in primary insomnia. Acta Neurobiol Exp. 2001;61:299–308.
- Anderer P, Saletu B, Saletu-Zyhlarz G, et al. Brain regions activated during an auditory discrimination task in insomnia post-menopausal patients before and after hormone replacement therapy: low resolution brain electromagnetic tomography applied to event-related potentials. Neuropsychobiology. 2004;49:134–153.
- Saletu B, Anderer P, Saletu-Zyhlarz GM, et al. Identifying target regions for vigilance improvement under hormone replacement therapy in post-menopausal syndrome patients by means of electroencephalographic tomography (LORETA), Psychopharmacology. 2005;178:389–399.
- Saletu M, Anderer P, Saletu-Zyhlarz GM, et al. EEG-tomographic studies with LORETA on vigilance differences between narcolepsy patients and controls and subsequent double-blind, placebo-controlled studies with modafinil. J Neurol. 2004;251:1354–1363.
- Anderer P, Klosch G, Gruber G, et al. Low-resolution brain electromagnetic tomography revealed simultaneously active frontal and parietal sleep spindle sources in the human cortex. Neuroscience. 2001;103:581–592.
*Dr Clete Kushida is the principal investigator of the Stanford study, which is part of a multicenter study—Airway Positive Pressure Long-term Efficacy Study (APPLES), National Institutes of Health (NIH), National Heart, Lung, and Blood Institute (NHLBI). Apnea Positive Pressure Long-Term Efficacy Study. Study ID number: 150; U01 HL068060. January 9, 2003. Or it can be accessed online at:clinicaltrials.gov/ct/show/NCT00051363; last accessed on June 28, 2007. Funded by the NIH. The Stanford study is still open to new subjects. Interested individuals need to live in the Bay Area and be 30 to 50 years old. Individuals can leave their name and phone number with Dr Olga Prilipko at (650) 723–7780 or contact the study at.