Sleep medicine has traditionally been the preserve of pulmonologists, but that’s changing thanks to physicians such as otolaryngologist-sleep specialist Brett Scotch, DO, FAOCO.
Sleep medicine is among the newest fields in medicine, but it is already steeped in its own traditions, including that it is primarily thought of as a subspecialty under pulmonology. But non-pulmonologists also pursue sleep medicine certification and can bring a fresh perspective.
One of those is sleep specialist Brett Scotch, DO, FAOCO. Scotch, also board certified in otolaryngology (also known as “ENT” for ear-nose-throat) and facial plastic surgery, provides a comprehensive approach to sleep medicine at the Scotch Institute of Ear Nose & Throat in Wesley Chapel, Fla. “By the numbers, it does appear that otolaryngologists make up one of the smallest percentages of certified sleep medicine doctors at the present time,” he says.
Though Scotch’s involvement in sleep medicine was the result of professional necessity versus a long-term professional plan, he is now an advocate and example of the benefits of an interdisciplinary approach to sleep medicine.
Hand of Fate

The Scotch Institute of Ear Nose & Throat in Wesley Chapel, Fla, provides a comprehensive approach to sleep medicine.
Scotch began his career as an officer in the US Air Force medical corps. He was an ENT, providing care to active duty military personnel, retirees, and their families. In 2006, fate intervened and set him on his path to sleep medicine.
When the staff sleep medicine physician received orders for deployment, Scotch was tapped to fill that role. After a year of intensive training and coursework, Scotch took over as the chief of sleep medicine and as medical director of a 2-bed sleep lab within the military treatment facility.
It wasn’t until 2007 that otolaryngologists could pursue sleep medicine as a subspecialty, so Scotch was ahead of his time.
Scotch recognized that his ENT expertise combined with his sleep medicine training let him provide comprehensive care to ENT patients who were struggling with sleep disorders. “I [was] able to provide my patients all options in treating their sleep disorder,” Scotch says. “Whether it’s a patient suffering from mild obstructive sleep apnea (OSA) who just needs a plan for success with weight loss or a patient with severe OSA who was intolerant to CPAP, the flexibility to shift gears to accommodate each patient’s unique treatment needs inspired me to subspecialize in sleep medicine. I love the diversity of sleep medicine and the reward that comes from helping someone achieve better quality sleep and better quality of life.”
Scotch was honorably discharged from the US Air Force in 2008 achieving the rank of Major. Among the decorations he received were the Meritorious Service Medal, the Global War on Terrorism Service Medal, and the National Defense Service Medal.
Scotch credits the training he received in the military as an ideal way to begin his practice both as an otolaryngologist and a sleep medicine physician. He also appreciates the bonds he forged with fellow physicians and patients. “When you’re serving our country in the armed forces, it’s truly a brotherhood,” he says. “I established relationships and bonds that will last a lifetime. Even today, I care for many of my former military patients as they have transitioned to civilian life. It was truly a privilege to serve some of the best and bravest airmen, marines, soldiers, and sailors as an ENT/sleep medicine physician while on active duty.”
A Natural Fit
As Scotch discovered during the early days of his sleep medicine career, medical professionals other than pulmonologists bring skills and knowledge to the treatment table to help patients.
According to Scotch, these include specialists in family medicine, internal medicine, pediatrics, otolaryngology, and neurology/psychiatry. All of these specialties are now eligible—with the appropriate training—to subspecialize in sleep medicine.
With the growing incidence of OSA in the general population, fueled, in part, by the epidemic of obesity, it seems only natural to Scotch that otolaryngology should play a part in the treatment of sleep disorders. “Otolaryngologists have always been the specialists of airway management,” he says. “So as the medical profession’s appreciation for and ability to appropriately diagnose forms of sleep apnea has increased, so has the need for the otolaryngologist trained in the appropriate management of the sleep apnea patient suffering from upper airway obstruction.”
This makes the otolaryngologist with a subspecialty in sleep medicine uniquely qualified to manage all aspects of a patient’s care in relation to disordered breathing, according to Scotch, including both medical and surgical options.
Setting Up Shop
[metaslider id=236033]
With his Air Force service complete, Scotch founded a solo ENT/sleep medicine practice in suburban Tampa, Fla. He also serves as medical director of a 5-bed independent diagnostic testing facility sleep lab near his office, and has hospital privileges in the sleep medicine and otolaryngology departments at several local hospitals where he also serves on the polysomnography interpretation panel.
In his clinic, Scotch treats about 1,000 sleep-disordered patients per year across the gamut of sleep disorders from OSA to narcolepsy. The treatment approach in the state-of-the-art multidisciplinary clinic is highly personalized, taking into account the patients’ health and lifestyle in the diagnosis and treatment of sleep disorders.
His patients appreciate having the entire array of treatment options at their disposal, Scotch says, noting that many are “very educated” about their sleep disorder and want a complete long-term treatment plan from weight loss and CPAP to surgical options, as necessary.
“Most of my patients are managed medically; however, I utilize state-of-the-art surgical options and technology available for my sleep-disordered breathing patients,” Scotch says. “Each patient’s needs are individualized; however, there is a subset of patients with obstructive anatomy that benefits tremendously from addressing intranasal or oropharyngeal obstructions.”
Among the surgical options that Scotch provides patients to alleviate their sleep-disordered breathing:
- For patients with massive tonsils and/or crowded oropharynx: tonsillectomy (sometimes combined with an adenoidectomy or uvulopalatopharyngoplasty).
- For patients with nasal obstruction due to nasal polyposis: nasal polypectomy (utilizing advanced 3D image-guided endoscopic technology).
- For patients with other types of intranasal anatomy: nasal septoplasty or turbinate reduction procedures.
- For patients with obstructive tongue bases or posteriorly positioned anatomy: hyoid and tongue base suspension techniques, tongue base reduction techniques using radiofrequency energy, palatal stiffing, and soft palatoplasty.
Many of the smaller, routine procedures are performed in Scotch’s clinic under local anesthesia.
For select patients with moderate to severe OSA who are unable to tolerate or receive consistent benefit from CPAP, an implantable hypoglossal nerve stimulator is an option that has shown significant benefit as well.
“It really helps to have all the tools of treatment at my disposal,” Scotch says. “It allows me to discuss a logical, stepwise progression of treatment with my patients from the outset. I educate my patients regarding their condition and lay out a road map for successful treatment from noninvasive, to minimally invasive, to more complex surgical intervention when required.”
In addition, Scotch performs outpatient sleep endoscopy to evaluate the dynamic nature of the airway in the sleeping patient under induction anesthesia. “With this additional knowledge of the patient’s complex and multidimensional pattern of airway obstruction, I can customize the patient’s operative intervention to the patient’s specific needs to increase the likelihood of success and possibly even minimize the scope of intervention,” he says. “Information garnered from sleep endoscopy sometimes proves that airway surgery would be less effective than desired, thus helping us determine who would not benefit from surgery.”
Among Scotch’s affiliations is with an ENT specialty outpatient surgery center, which is staffed by anesthesia staff with an interest and appreciation for patients with sleep-disordered breathing conditions. “I routinely collaborate with my anesthesiologist in preoperative screening and postoperative referral process for patients at high risk of OSA,” he says. “In addition, upon anesthesia induction, signs of OSA often become apparent, prompting our collaboration to benefit the patient with early identification and treatment.”
Collaborative Approach
Perhaps a legacy of his military medical career, Scotch practices a highly collaborative approach to sleep medicine, which adds to the benefits of the one-stop treatment approach that is provided by Scotch’s clinic.
“In my practice and affiliated sleep lab, we utilize a collaborative approach between multiple specialties to include pulmonology, neurology, psychiatry, and otolaryngology,” he says. “This multidisciplinary approach to care allows the physicians to share an electronic health record platform where we can all seamlessly access patients’ sleep history, PSG and PAP studies, records, questionnaires, and DME [durable medical equipment] orders. When we need to obtain additional specialty opinions on complex cases, having this collaborative, connected network of professionals is a tremendous benefit to the patient. Our sleep patients have their conditions diagnosed and treated expediently, efficiently, and with comprehensive multidisciplinary follow-up care.”
Kathleen Racich, DO, has worked with Scotch since he set up practice in 2008. Racich, who specializes in neuropsychiatry, says her holistic approach to patient care is what fundamentally links her and Scotch’s practice.
“If you look at psychiatric disorders in general, such as anxiety, or depression, or bipolar disorder, often there is an underlying sleep disorder. They’re miserable because of their mood symptoms, so sleep disorders are often overlooked,” she says. “I’m really holistic in my approach.”
This holistic approach dovetails with Scotch’s collaborative practice. Racich notes that while she may be focusing on her patients’ mental health, every aspect of her patients’ health is her concern. This includes looking at sleep.
If she suspects that one of her patients has an underlying sleep disorder, such as OSA, she will refer them to Scotch who will evaluate and if necessary treat the patient.
Treating a sleep disorder might be a key aspect of helping the patient’s psychological issues, Racich says. “If my patients aren’t [medically] perfect, then what I do won’t work,” she says.
This collaborative approach has numerous benefits for all the patients Scotch and his colleagues see, including better outcomes and better communication between the ENT surgeon and anesthesiologist regarding the patient’s condition and details of the precarious airway prior to the patient being anesthetized.
A Multidisciplinary Future?
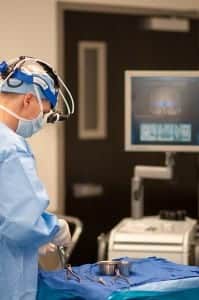
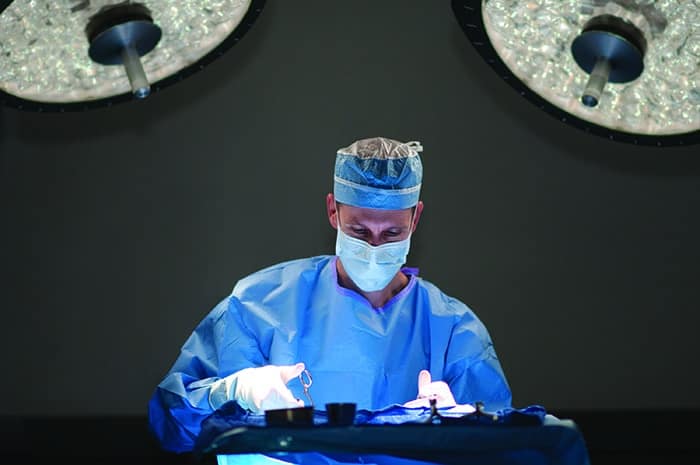
Scotch collaborates with other specialists, such as pulmonologists,
neurologists, and psychiatrists to care for patients with sleep disorders.
While certainly an ideal, is Scotch’s approach to sleep medicine its future? Scotch certainly thinks so.
“I think that the multidisciplinary approach to care is a viable option for today’s sleep center,” Scotch says. “It does require a willingness to collaborate in care and an appropriate team needs to be assembled and focused around the common goal of achieving increased longevity and better quality of life for our patients.”
In addition, Scotch says that as more physicians enter the field from other specialties, it is translating into increased access, improved patient care, and better outcomes. “The face of sleep medicine is changing and the scope of knowledge is ever increasing,” he says.
And Scotch knows this first hand. As an advocate of increasing the specialties involved in sleep medicine, he notes that ENTs have the ability to handle the most complex of sleep disorder cases. “I think the ENT/sleep medicine physician fills an important niche in treating patients with sleep-disordered breathing conditions, snoring, and other sleep issues. As part of a collaborative team, we can do the most good by partnering with our pulmonary, internal medicine, family practice, pediatric, neuropsychiatric, and anesthesia colleagues for optimal patient outcomes,” he says. “Typically, most don’t know of the ENT’s role in sleep medicine, but I think with increased education of what we do, that will evolve over time to benefit more patients.”
Having seen a few ENT physicians in his early life and having written for Sleep Review magazine since 2001, Los Angeles-based freelancer C.A. Wolski was surprised he never made the connection that ENTs are a natural fit as sleep medicine physicians.



![ProSomnus Sleep Technologies Launches ProSomnus [CA] LP Continuous Advancement Sleep Device](https://sleepreviewmag.com/wp-content/uploads/2019/12/ProSomnus_CA_LowProfile_HERO-440x264.png)
I just wanted to say Dr.Scotch is the most caring Dr. That I have ever seen, he is awesome in every field he has done so much for me rather it was surgery on my ears and the care for them to removing moles on my face . Unfortunately my insurance changed and he did not take that insurance. I miss him so much . Dr. Scotch thank you very much for everything you did for me. You are the best . Thank you