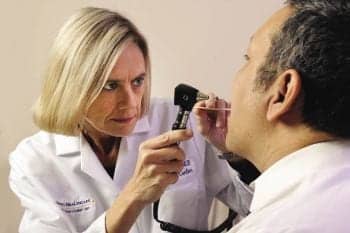
Photos by Jack Kearse

Nancy Collop, MD, got her first taste of sleep medicine working with Anthony Kales, one of the field’s pioneers, who, along with Allan Rechtschaffen, published the first manual on how to score sleep stages in 1968. A student at Pennsylvania State University College of Medicine at the time, she had a work-study job in Kales’ sleep lab. A few years later, while doing her fellowship in pulmonary/critical care at the University of Florida, she found herself working with another leader in the sleep field: A. Jay Block, MD, whose early work provided the foundation for future research on respiratory monitoring during sleep and is credited with describing a hypopnea. Since that time, Collop has become a leader in the field of sleep medicine herself, most recently as president of the American Academy of Sleep Medicine (AASM).
With more than 20 years of experience in the field, Collop has gained the respect of her colleagues who welcome the fact that she brings the best of both worlds to the field of sleep medicine, combining an academic and clinical background that serves her practice and the field as a whole.
“Often you see a doctor who is strong on either the academic side or the patient side—bedside, if you will. But seldom do they have both skills,” says John H. Mathias II, president of Sleep Services of America, a GE Healthcare Company, who worked with Collop at Johns Hopkins where she was the medical director of the Sleep Disorders Center. “Nancy has a wide breadth of experience. She has practiced in the north and south, and in small and large institutions. She worked in the Veterans Administration system. She comes from so many different touch points that I think it’s easy for her to understand [the concerns of differing communities].”
In addition to working at Johns Hopkins, Collop has held academic positions at the Medical University of South Carolina and the University of Mississippi. In 2010, she left Hopkins to take on the opportunity to develop a sleep center at the Emory School of Medicine in Atlanta. Currently, she serves as director of the Emory Sleep Center and holds a primary appointment as professor of medicine in the pulmonary, allergy, and critical care medicine division and a secondary appointment as professor of neurology. The move to Emory, as she puts it, allows her to do “100% sleep medicine now,” including an active clinical program where she sees patients.
AASM PRESIDENCY

Nancy Collop, MD, evaluates a patient’s polysomnography results to determine treatment options. The integrated sleep management model aims to keep the sleep specialist engaged throughout a patient’s care.
Currently, that 100% focus on sleep also includes serving as AASM president until June. When Collop stepped into her role, one of her goals was to further raise public awareness among the public, hospitals, and physicians about sleep and its role in overall good health. But another one of her goals may be more challenging and have a more lasting impact on the future of the field.
As AASM president, Collop finds herself trying to figure out the future of sleep medicine and, more specifically, how sleep medicine is going to fit into health care reform. Her goal is to keep the organization and its members ahead of the curve. And right now, that work boils down to the AASM’s recent proposal to the Centers for Medicare and Medicaid Services (CMS) for an integrated sleep management delivery model.
PATIENT-CENTRIC CARE
The impetus for work on an integrated model grew out of CMS’ 2008 work on home sleep testing (HST) payment, when, according to Collop, some of the agency’s own language implied that they really wanted someone to find a way to integrate care in sleep medicine. At the same time, the AASM wanted to make patient care less fragmented, while also making it more outcomes-oriented. And while a recent letter to AASM members indicated that the Academy was “keenly aware of the challenges facing the field of sleep medicine” and the necessity of finding new opportunities to “stay competitive” amid cuts to payments, Collop maintains that better patient care is at the heart of this initiative.
The integrated delivery model starts with a patient referral to a sleep specialist who decides the patient’s treatment pathway. The specialist first will make the decision as to whether a patient needs a sleep study. If the patient is suspected to have sleep apnea, the physician will determine the most appropriate test (HST or polysomnography) for that individual, with consideration given to comorbid disorders that may make one test more appropriate than another. Following the test, and depending on the results, the sleep specialist then decides, along with the patient, the best form of treatment, whether that be CPAP, a dental appliance, surgery, or some other more conservative treatment. Within the context of this model, not only would the sleep specialist provide the durable medical equipment (DME), but they would also have a network of dental sleep medicine and surgical specialists to whom to refer patients. Having these established relationships and direct access to DME would close the treatment loop, creating a more seamless management process that keeps the sleep specialist at the center with the patient. Under the proposed model, patients would be followed for 2 years and outcomes evaluated. During this time, their treatment would be monitored to ensure not only compliance but better health.

Nancy Collop, MD, (right) discusses treatment options for sleep apnea with a patient. Maintaining a relationship with the patient throughout care is a key component of the integrated sleep management model.
“From my perspective, I think the management of the patient is the foremost reason to go this way. I struggle against this all the time in my practice, trying to get patients through the system and making sure they don’t get dropped. Patient first is always the way to go, but, certainly, we also have to be paid for what we do. So you can’t really do one without the other,” says Collop.
Under the current system, patients are getting lost between sleep centers and DME providers. The sleep doctor is often completely removed once CPAP is prescribed. While this fragmentation was seen as a way to prevent abuse from providers trying to game the system for financial gain, it has left patients floundering. As a result, Collop and her colleagues see patients who underwent a sleep study several years earlier, were diagnosed with OSA, and given CPAP with no follow-up. These patients end up in Collop’s office telling her a story she hears over and over again: ‘They gave me one of those CPAPs, but I didn’t really like it and never used it. But now I’m worse, so here I am.’ Complicating the issue further is the growth of HST use. The fact that doctors requesting a sleep study often are not the ones to make the decision as to what type of sleep test is administered leaves the patient alone, with no one actually seeing to it that they get the right sleep study or follow-up care.
The integrated model proposed to CMS this past September seeks to rectify this, creating a patient management system that stays with the patient from beginning to end.
By maintaining the patient’s relationship with the sleep specialist, the specialist, for example, can assess whether CPAP is the right treatment and, if not, look at other options, such as a dental appliance or surgery.
“We’ve heard a lot over the last 2 years that we should be tracking patients’ [health outcomes], not just how much they use their CPAP; but the way the system is set up, we don’t really track that,” says Collop. “We should be tracking whether they’re actually getting better, whether it’s preventing them from having a stroke or a heart attack, or developing diabetes.”

After agreeing with the patient that CPAP is the best treatment option, Nancy Collop, MD, (center) observes as sleep tech Cheryl Pallone, RPSGT, CRT, fits the patient.
The AASM’s current proposal to CMS was designed around the diagnosis and management of OSA, as the disorder has high health care costs and a high prevalence. The AASM fully intends to create something similar for other sleep disorders such as narcolepsy and insomnia, because this type of model and the work the AASM is doing aren’t about one disorder, but about sleep medicine as a whole, says Samuel A. Fleishman, MD, president-elect of the AASM and medical director of behavioral health and The Sleep Center at Cape Fear Valley Health System in Fayetteville, NC.
Fleishman agrees that the focus on integrating patient management in this model is appealing. “The field of health care in general is really asking for more integration, more comparative effectiveness, asking for more outcomes-based medicine,” he says. “If you look at sleep apnea in particular [under the current model], you have as many as three or four people trying to treat the patient and the patient going to three or four different places. Ideally, for the patient, they would come to one place to get evaluated, treated, and follow-up care.”
Mathias is excited by the prospect of such a model being implemented and the improvement it could bring to patient care. “What I’ve seen over the years is a difficult patient experience when it comes to sleep. [This] integrated model reduces touch points for the patient and adds more standardization for the patient. It is more outcomes-driven, which is better for the patient.”
IN PRACTICE
According to Collop, the Emory Sleep Center where she practices is currently trying to implement elements of this model. “We have tried to make sure that every patient who has a sleep study knows the results. We do allow for direct referrals for sleep tests, but even with those patients, we try to get them into our clinic to do the results of the sleep test and make recommendations for therapy. So, from that perspective, we are trying at minimum to improve the care of the patient.”
And while the Emory Sleep Center does not have its own DME company, Collop says she has worked to cultivate relationships with DME companies and has given them guidelines as to what she requires for particular patients.
Currently, it remains to be seen whether CMS will embrace this model as a pilot project of its Innovation Center or go back through CMS’ rule making since such a model cannot function under current CMS rules. So far, Collop says the AASM has received “pretty positive feedback” from CMS and the few payors who have seen it, and hopes that they will continue to support the proposal and help flesh it out.
THE HURDLES
While CMS’ final decision remains unknown, there are a number of issues to tackle and problems to be ironed out. The proposal itself suggests that the model be trialed at test locations. In addition to having AASM accreditation for their sleep center, a DME program, and an out of center sleep testing program under the model, these test locations would need to have partnerships with dental sleep medicine professionals experienced with oral appliance therapy and surgeons experienced in upper airway surgery to treat OSA; they also would need a tracking mechanism for recording patient follow-up and outcomes, and a compliance program designed to prevent fraud and abuse. But even more difficult hurdles could impede moving the proposal forward. Collop concedes that it remains to be seen how HST and DME companies would fit into the model. In addition, many have wondered what role primary care physicians would play in the model.
Currently, some sleep centers have AASM DME accreditation, but not all patients can be accommodated through these labs—especially since AASM is not a deemed CMS authority. And while the AASM would like to change that, Collop admits there are some labs that don’t want to or can’t take on the DME component. “In that situation,” she says, “what we’ll be looking for is partnering with DME companies to really develop a stronger relationship, because the ultimate key is for them to provide the CPAP, but for us to monitor the patient’s care.” The goal, says Collop, is for all parties to have all the information needed to take care of the patient appropriately.
With regard to primary care physicians, Collop says the AASM envisions established relationships between these doctors and sleep centers. The sleep center could even work with them to perform a home sleep test through the primary care physician’s office, she says.
Moving forward, Collop admits there is still work to be done to determine how sleep professionals will be paid under this model, since testing is often the “big income driver.” In addition, payors must be convinced that this model will actually save them money in the long run. As Collop points out, if patients are managed under such a system, and effective treatment is undertaken, then the risk of stroke and uncontrolled blood pressure is diminished. Patient health can be improved, leading to lower health care costs in the long run.
While the AASM submitted a letter of intent to CMS in December and will submit a full application by the end of January, Collop points out that the proposal is still a work-in-progress and focus groups are ongoing, thus people should not read too much into it.
“The devil may be in the details with how it works out, but our goal is to continue to push something like this forward,” says Collop. “Our emphasis is on keeping the patient at the center of the model. And as long as the patient is not just getting the test, as long as the patient is cared for, we’re open to working with whomever.” And while the end result may or not be this model, Collop contends that “no matter what we do, it will be something like this.”
Currently, this is a model for Medicare patients, but down the road, if private payors take an interest, there will be a need for sleep centers, sleep doctors, and sleep technologists throughout the country to get behind the proposal to move it forward, says Collop, whose leadership on this has been key to moving it ahead.
“She has done a lot of work on this proposal to bring it forward,” says Fleishman. “She has a good idea of what kind of protocols [are needed], how patients should flow through the system, how diagnosis and treatment can be broken down, and efficiencies that can be utilized. She certainly is committed to this, to trying to get outcomes-based medicine moving forward, and to a patient-centered medical model.”
Mathias is watching to see where this model goes. “I don’t know what the outcome will be, but it will be a better model,” he says. “We all need to just stand back and give it a good shot and see if we can improve patient diagnosis and care as a result of this model.”
And Collop’s advocacy of a patient-centered model doesn’t surprise Mathias. “Nancy always seems to say, ‘Well, let’s look at the patient first.’ The patient comes first and the business comes second. I think that’s important in our industry today because there is so much rapid change.”
And Collop is doing her best to be one of the leaders who helps the field transition and adapt to this change.
Alison Werner is associate editor for Sleep Review. She can be reached at [email protected].