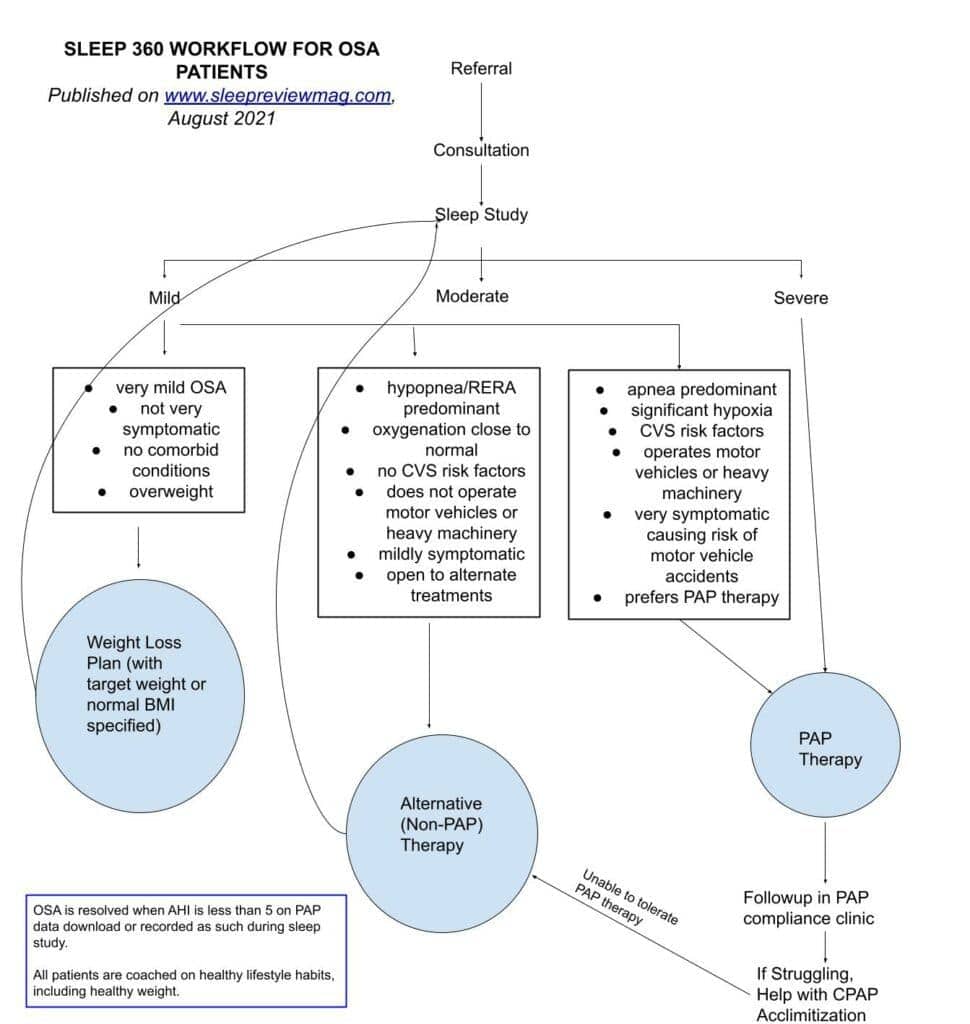
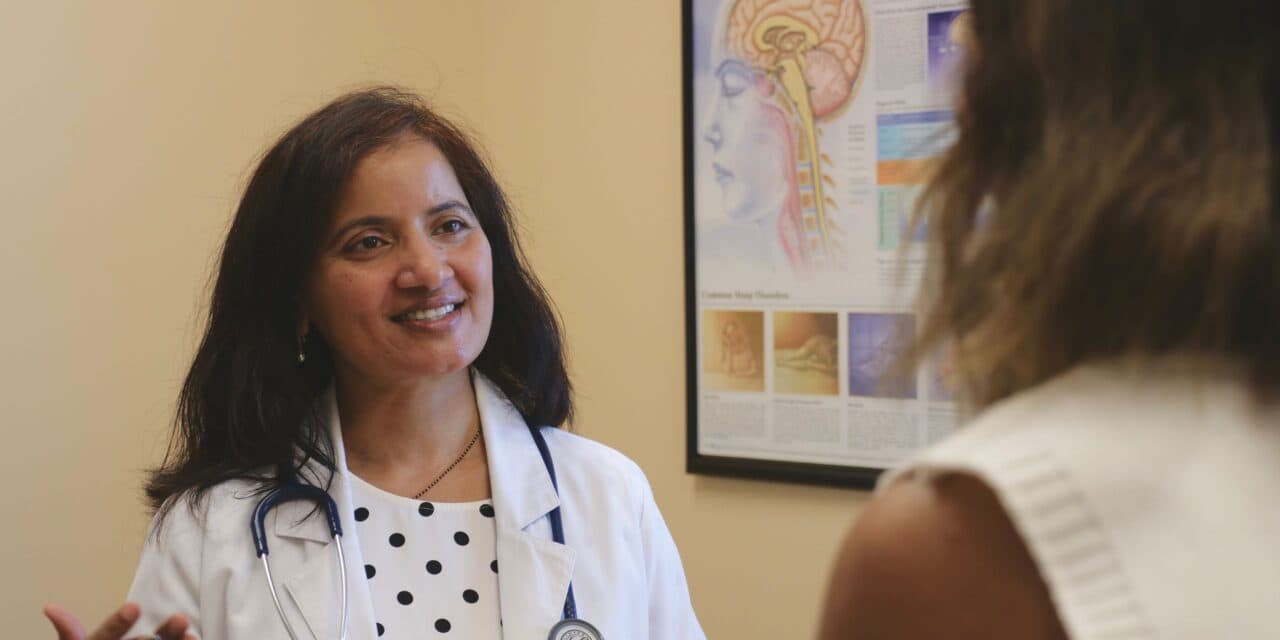A flow chart from Sleep 360 Sleep Diagnostic Center illustrates the OSA patient journey from referral to customized therapy.
By Vani S. Vallabhaneni, MD
A multidisciplinary approach is recommended for evaluating and treating obstructive sleep apnea (OSA), a chronic medical condition that is characterized by recurrent episodes of partial or complete upper airway obstruction during sleep. Untreated OSA is associated with increased cardiovascular morbidity, neurocognitive impairment, motor vehicle accidents, healthcare utilization, and all-cause mortality, all of which emphasizes the need for effective long-term treatment.
At Sleep 360 Sleep Diagnostic Center, our approach is to discuss all the treatment options, not only the common firstline therapy of positive airway pressure or CPAP therapy, and personalize each patient’s treatment plan from the start. We work closely with a variety of specialties, including dentistry, oral-maxillofacial surgery, and otolaryngology for the best patient outcomes.
Although CPAP is highly efficacious in preventing upper airway collapse, challenges with it include patient acceptance, tolerance, and adherence—thereby reducing effectiveness. What’s more, some patients using CPAP are looking for more convenient options during travel, while another subset wants a permanent non-PAP-based solution. There is a dire need for effective alternative treatments.
At Sleep 360, we approach patients as a whole, assessing their cardiovascular risk profile and symptoms, for example.
- Are they very symptomatic with a high risk for motor vehicular accidents?
- Are they unable to perform at work due to sleepiness/fatigue/tiredness?
- Are they in a job that includes operating heavy machinery or are they a commercial truck driver or pilot?
- Are they only mildly symptomatic or is OSA impacting their personal life?
- What are the specific characteristics of their OSA?: Are they apnea or hypopnea or RERA predominant, what is their oxygen desaturation index, how much time are they spending below 90% oxygenation, is there resting tachycardia?
- What are they willing to use to treat their sleep apnea?
- Can they afford the treatment, as some of the alternate treatments are not covered by insurance plans?
A flow chart of the Sleep 360 workflow illustrates how we take these and other factors into account.
Alternative therapies that we discuss with patients include the following.
Mandibular Advancement Splint/Mandibular Advancement Device/Oral Appliance (OA)
An update on Clinical Practice Guidelines from the American Academy of Sleep Medicine (AASM) and American Academy of Dental Sleep Medicine (AADSM) for the Treatment of OSA and Snoring with OA Therapy was published in 2015. They recommended customized, titratable OA devices by certified dentists as a treatment for adult patients with OSA who cannot tolerate CPAP or who are looking for an alternate treatment. The patients should have a follow-up sleep study using OA to verify resolution of OSA. The dentist and sleep physician should provide follow-up care to monitor for any side effects from treatment.
OA are used for the treatment of OSA both as a primary therapy for mild and moderate OSA and as an alternative for patients with severe OSA who are unwilling or unable to tolerate CPAP. OAs are a simple, reversible, quiet, and cost effective therapy for selected patients with OSA. There was no significant difference between OAs and CPAP in the percentage of mild OSA patients achieving their target apnea hypopnea index (AHI)/respiratory disturbance index/respiratory event index (<5, <10, >50% reduction) after treatment. For patients with moderate to severe OSA, however, the odds of achieving the target AHI were significantly greater with CPAP than with OAs.
The challenge has been to identify OA responders and non-responders prior to initiation of therapy. In a small study, CPAP pressures above 13 cm H2O (in Caucasians) and 10.5 cm H2O (in a Japanese population) are likely to indicate non-responsiveness to OA treatment. However, prospective validation of CPAP pressure as a predictor of OA response is still required.
A recent comprehensive review of OA treatment showed a response rate of OA can range from 29% to 71% with complete response noted in 48% of patients. In upper airway endoscopy, the cross-sectional area of expansion at velopharynx was much greater in OA responders versus non-responders with a high level of predictive accuracy (sensitivity of 85.7%, specificity of 80.8%, positive predictive value of 85.7%, negative predictive value of 80.8%) was found with a cut-off value of 2.0. To put this to practice, during OA titration, it’s best to aim for a mandible position where the velopharynx is visually widened by two times compared to chin rest position. This reduces collapsibility of the upper airway and side effects from excessive mandible protrusion including temporomandibular joint disorder and other muscle and teeth problems, thus improving compliance and efficacy.
Many patients can effectively use OA as a short-term treatment alternative to CPAP for travel with satisfaction rates reported up to 75% with no significant differences in SAQLI (Sleep Apnea Quality of Life Index) between OA and CPAP treatment.
Hypoglossal Nerve Stimulation
Inspire is a pacemaker-sized implantable pulse generator that senses chest wall movement during sleep. It treats OSA by stimulating the hypoglossal nerve resulting in contraction of the genioglossus muscle, which protrudes the tongue and enlarges the retrolingual and retropalatal levels of upper airway, addressing this neurofeedback-loop dysfunction seen in OSA patients. Inclusion criteria include being 18 years of age or older, having moderate to severe OSA with an AHI of 15/hr to 65/hr, a body mass index less than 32, and absence of concentric retropalatal collapse of upper airway during a drug-induced sleep endoscopy. Early studies of the efficacy of hypoglossal nerve stimulation showed that AHI decreased by 68% 12 months after implantation, with improvement in daytime sleepiness and quality of life. Four-year follow-up results indicate ongoing effectiveness of therapy with regard to subjective measures of quality of life.
Uvulopalatopharyngoplasty (UPPP)
It used to be the most common surgical approach, aimed at removing excessive tissue in the upper airway, but the overall success rate of UPPP has been reported to be around 40% due to poor patient selection. Sleep video fluoroscopy has revealed that measurement of the mouth-opening angle could predict surgical outcome with predictive values of 72.4% and 82.5% for success and failure, respectively.
Evaluation and surgical correction of upper airway anatomical abnormalities such as deviated septum, nasal polyps, tonsillar hypertrophy, excessive parapharyngeal fat, and enlarged turbinates can improve nasal patency and PAP tolerance by reducing average pressure requirements on CPAP.
Maxillomandibular Advancement, Genioglossus Advancement
Although maxillomandibular advancement is typically reserved for select patients with moderate to severe OSA, genioglossus advancement alone may have utility in select patients with mild or moderate OSA. These procedures expand the facial skeleton anteriorly and displace all associated soft-tissue and muscle attachments to achieve multilevel (via maxillomandibular advancement) or retroglossal (via genioglossus advancement) expansion of the upper airway. Negative postoperative alterations in facial appearance are typically minimized by selecting patients with a retrognathic maxillomandibular complex and undersupported or lax facial soft tissues.
Expiratory Positive Airway Pressure (EPAP)
Bongo Rx is an FDA-cleared EPAP device to treat mild to moderate OSA with predominant hypopneas. Patients with no cardiovascular risk factors are suitable candidates for Bongo Rx. It is reusable, travel-friendly, easy to clean, small enough to fit in a shirt pocket, and does not require a hose, mask, or electricity source. It is available in a starter kit with 4 sizes or in an annual pack. In a clinical study, nasal EPAP significantly reduced AHI, improved subjective daytime sleepiness, and reduced snoring—with excellent long-term adherence in those who had a positive clinical response at 3 months.
Positional Therapy
Patients with positional OSA have lower CPAP adherence and CPAP treatment may not be optimal. There are a variety of devices, including tennis balls, body positional belts, and vibrating devices to keep a patient off their back. They have shown good results in the short term but long-term compliance is limited because of complications and low satisfaction in some patients. At a 6-month follow-up, only 35/84 patients (41.6%) were regularly using the device, with a mean of 5.9 ± 1.2 days per week.
ExciteOSA
The eXciteOSA device works by delivering electrical muscle stimulation through a mouthpiece that sits around the tongue. The mouthpiece has four electrodes, two located above the tongue and two located below the tongue. It is used for 20 minutes once a day during a wakeful state for a period of 6 weeks and once a week thereafter. Patients should receive a comprehensive dental exam prior to use. The eXciteOSA device is contraindicated for patients with pacemakers or implanted pacing leads (electrodes); patients with temporary or permanent implants, dental braces, intraoral metal prosthesis/restorations/appliances, or dental jewelry in the mouth; patients who are pregnant or may be pregnant; or patients who have ulcerations in or around the mouth. The eXciteOSA device is not intended for patients who have or are suspected of having OSA with an AHI of 15 and higher.
In conclusion, based on the global picture, we discuss the best treatment approach with our patients. We follow them closely and if they have clinical improvement on therapy, we do a follow-up sleep study to make sure they are optimally treated. If not, we discuss other treatments or combination therapy. We highly stress weight loss by lifestyle changes in our patients who are overweight or obese. We educate them about food choices, mindful eating habits, and the importance of routine exercise. We do a follow-up sleep study to see if their sleep apnea has resolved after they reach their target weight. We also educate them about healthy sleep habits, including having 7 to 9 hours of sleep nightly to have the best outcome for their OSA therapy.
Our success is reflected by personalizing and optimizing the treatment to patient needs.
Vani S. Vallabhaneni, MD, is founder and medical director of Sleep 360 Sleep Diagnostic Center, established in 2008, in Austin Texas, an American Academy of Sleep Medicine-accredited sleep center providing comprehensive solutions and continuity of care for patients with sleep problems. She has served in various capacities at her county medical society and Texas Medical Association, currently serving as a delegate of her county medical society to Texas Medical Association. She has a keen interest in sleep research. She is a co-investigator in a National Institutes of Health-sponsored multicenter prospective study—“Memories 2”—to understand the relationship between obstructive sleep apnea and mild cognitive impairment.
Top photo: Vani S. Vallabhaneni, MD, founder and medical director of Sleep 360 Sleep Diagnostic Center, takes pride in working collaboratively with other specialists to provide optimal and personalized care for patients.