Michael Zachek, MD, has embraced home sleep testing for obstructive sleep apnea—and so have potential patients. In Bowling Green, Ky, The Graves Gilbert Clinic’s seamless process ensures more people start therapy within a week of their first appointment.
If “Advantages of Home Sleep Testing Over In-Lab Testing” appeared as a survey question on Family Feud (albeit, a peculiarly healthcare-focused episode), the game show board would certainly include the answer “easier for the patient.” At The Graves Gilbert Clinic in Kentucky, Michael Zachek, MD, wins points with patients as he utilizes home sleep testing (HST) to get more people with obstructive sleep apnea (OSA) from appointment to therapy quickly.
In 2012, the year immediately before adding HST, The Graves Gilbert Clinic completed 1,300 sleep studies (all in-lab). In the most recent year (2016), the clinic did 2,000 sleep studies total—a 54% increase. Of those, about two-thirds were HSTs—“HSAT”s, home sleep apnea tests, as the clinic more specifically refers to them—and the lab beds were still used for about 700 polysomnograms (PSG) and CPAP titrations. The volume of studies done at The Graves Gilbert Clinic is aspirational for many sleep labs.
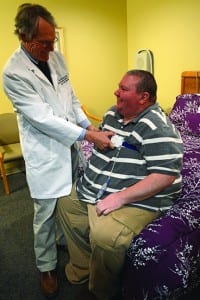
Zachek’s team spends time instructing patients (in this photo, depicted by an employee) on how to put on an HST device correctly, even providing them with YouTube how-to video links.
Finding His Niche
Zachek, director of the physician center for sleep disorders at The Graves Gilbert Clinic, is board certified in internal medicine, pulmonary disease, critical care medicine, and sleep medicine. Graves Gilbert is a multispecialty clinic with about 150 providers including 50 primary care clinicians, has most specialties in house, and Zachek is one of six physicians who practice sleep medicine there (and the only one who practices it exclusively). It has a total of 10 sleep center beds at three locations.
Zachek is also director of sleep at Ohio County Hospital and at Twin Lakes Regional Medical Center. He is a site visitor for the American Academy of Sleep Medicine (AASM), as well as an AASM Gold Standard Scorer.
With his many titles and accolades in sleep medicine, one could be forgiven for making the assumption that Zachek has focused on the subspecialty his entire career. In reality, he did not learn sleep medicine until he was already a busy pulmonary and critical care doctor. “I had no formal sleep training because there was no such thing as sleep training during my internship and residency,” says Zachek, who in 1980 completed his internal medicine residency at Duke University. In 1982, when he completed his pulmonary fellowship at Washington University in St. Louis, sleep disorders were just starting to become recognized in a real-world way, he recalls. He also lived and worked at several U.S. Air Force bases, but did not do any sleep studies there, also due to the timing.
So it was the early 1990s when Zachek began doing sleep studies as part of his pulmonary/critical care practice. “I was self-trained,” he says. At first the sleep disorders patients were occasional. But ultimately Zachek found sleep medicine more satisfying than pulmonary or critical care. So in 2007, he became a sleep medicine physician full-time. “What pulmonary and critical care physicians treat—COPD, lung cancer, etc—are chronic, debilitating conditions. In general, even if you’ve done the best job you can, most of these people at some point deteriorate. You lose a lot of good friends in pulmonary,” he says. “With sleep, I am rewarded every day. Patients regularly tell me, ‘Doc, you’ve changed my life and I feel so much better.’”
For about two decades, all of the sleep studies he conducted were in-lab. His clinic added HSTs in 2013, and Zachek still prefers HST devices that incorporate PSG-utilized transducers. “From my mindset, I’m looking at PSGs regularly. I like the idea of looking at the same kind of sensor when I read a home sleep apnea test,” he says. Graves Gilbert rents its HST devices, because they find it less expensive for the high volume of patients, as well as because any repairs remain the responsibility of the device owner.
[metaslider id=198387]
Testing the HST
At the end of 2012, when Anthem became the first payor to advise The Graves Gilbert Clinic that it was going to begin insisting that certain patient populations be tested via HST, Zachek was prepared. “As a site visitor for AASM, I’d been preaching [HSAT preparation] for a year. I’d seen it and had told other centers about it,” he says.
Zachek had the foresight to test the modality at his sleep lab prior to any payor requiring him to use it. “To convince myself this was an appropriate modality for testing, we actually had 50 people sleep in our main sleep center and undergo a full polysomnogram, but we also put the home sleep apnea testing device on them. They did both tests at the same time. I analyzed that information, though I never published it, and our results suggested it was a pretty good test,” he says. His study found a correlation coefficient of 87%. Even better, for the population he typically saw—those with moderate to severe OSA—the HSTs had an even stronger correlation. “So by the time [payors] told me they would only pay for home sleep apnea tests, I felt confident that we were good to go,” Zachek says.

The Graves Gilbert Clinic has 10 sleep lab beds total—six at its main location and two each at both satellite clinics. The beds are still used several nights every week for in-lab sleep studies, though not as much as they were prior to the clinic incorporating HST in 2013.
Easy As 1-2-3
Gaining patient acceptance for HST was easy because the test was so much more convenient for patients than an in-lab study. After the clinic added HST, Zachek says the biggest surprise was “how many patients wanted to be seen for sleep problems that were reticent about being evaluated previously.” Prior to HST, common reasons patients gave for not completing sleep studies included, “I don’t want to sleep away from home,” “it’s too expensive,” and “it takes too long to get into the lab.” Now they get a study and are on therapy within about a week. “When you make it easy for people, it makes it more likely for them to follow through on the evaluation and treatment,” Zachek says.
Zachek made it even easier by removing common interruptions that would traditionally cause patients to lose momentum in their diagnosis to treatment journey. For example, he eliminates the delay between the patient taking the study and receiving its results. Once a patient is determined to need a sleep study, Zachek tells him or her to pick up the device the night before the patient’s next scheduled appointment in order to complete the study literally the night before Zachek is scheduled to read it. He tells patients to “bring the completed test in the next morning, and to bring something to read because we’re going to score it while you wait.” He then reviews the study and gives the patient a CPAP prescription (if needed) that day—so less than 12 hours from when the patient strapped on the effort belts and inserted the nasal cannula, he or she has prescription in hand.
Zachek also eliminated delays that can arise on the DME’s end. One way he accomplished this is by making all DMEs “pharmacies” in the clinic’s electronic health records (EHR) software. “So I can prescribe CPAP in my EHR and send orders directly to the DME like a prescription,” he explains. So the DME already has the documentation it needs, and the patient is given a business card for the DME of their choice and told to contact the DME that day to pick up the CPAP (Zachek ensures all DMEs they work with provide him with plenty of business cards). “We’ve worked out which DMEs give us good service and which do not. We don’t give our business to those who take a week to fill a CPAP order. I want my patient on therapy today,” Zachek says. Starting CPAP the same day as the OSA diagnosis is analogous to a patient diagnosed with pneumonia expecting to start antibiotics the same day. After all, “if the DME takes a week to set you up, it couldn’t have been that important a problem,” he says—an incorrect and inaccurate (though common) representation of the seriousness of OSA.
Most patients start therapy on auto-PAP, but Zachek soon thereafter determines a fixed pressure setting. Patients typically either get a CPAP device that has a trial auto-adjusting mode or purchase an APAP but use it as a CPAP once their therapeutic pressure is determined.
Zachek continues to be involved to ensure any adjustments are taken care of expediently. “With the advent of modems, we tell the patients to see the DME if they need a mask change, but if they have a pressure problem, call me and I’ll look you up and make the change in prescription right then,” he says. “So when they come back in for their next appointment, they’re on therapy and they’re doing well.”

Several sleep team members at The Graves Gilbert Clinic pose for a photo. From left to right: Jason Fulton, RPSGT, Kelly Hunter, RPSGT, Charity Casavechia, LPN, Joan Douglas, APRN, and Zachek.
Handling the Cascade of Changes
Of course, incorporating a higher volume of HSTs has other consequences for the sleep center too. “We do fewer nighttime studies. I used to run 6 nights a week; now we run 4 nights a week, so I’m spending money [on the space] for 3 nights I don’t use. If I were to build a new one, I’d have a smaller footprint with four beds,” Zachek says.
Fewer nighttime studies means fewer nighttime techs are needed, but at The Graves Gilbert Clinic this has not resulted in layoffs. Instead, “we allowed them to do other jobs,” Zachek says. For example, techs now score sleep studies during the day since that’s when patients bring in their HSTs. Also techs help instruct patients on how to put on the HST devices to lessen the risk of incomplete tests. Some staff also sought additional training in order to transition to other open positions at the clinic.
Staffing and appointment modalities have also adjusted accordingly with the higher volume of patients who are on therapy and thereby need follow-ups and rechecks. Specifically, Zachek started with one nurse practitioner; he now has three (including a new hire at a satellite clinic). He also incorporates telemedicine for recheck appointments (never for the original appointment) for patients in rural areas. “I sit with them via telemedicine and…that’s been very helpful for my patients. They don’t have to wait so long for an appointment. I can see patients more efficiently because I’m sitting in one place,” Zachek says, adding, “You don’t bill as much [as you would in person] but then you’re not doing as much either.”
Removing Final Barriers
HST allows Zachek to diagnose and treat more patients with OSA, but it’s likely he could see patients even more efficiently if payors would remove prior authorization requirements for home sleep tests. “It would be really nice if insurance companies would recognize that this low-cost test should performed without authorized as it’s about the same price as routine x-rays that don’t require authorization,” Zachek says.
He says it would be more time effective if payors only required prior authorization for PSGs, noting that he cannot recall the last time he received a payor HST denial. Sleep center staff spend on average 30 minutes on the phone (or online) to request prior authorization for every patient. That seems like a particularly poor use of time. “If I can save a half hour on a patient, that’s time when our staff could do something else,” Zachek says. “Some of the prior authorizations for HST even take up to 14 days”—time during which the patient may be losing momentum and interest.
Zachek does agree with payors on documentation requirements; for example, he gives patients a nine-page sleep questionnaire, which he reviews and stores in the EHR. He says the documentation would continue to remain available to the payor, if it wished to audit records for the appropriateness of the study.
For patients who need in-lab testing (such as due to comorbidities), by carefully documenting the reasons for a PSG, Zachek is typically able to get authorization from payors. About four times in the past year he has needed to speak directly with a payor’s medical director to get the authorization (typically he accomplishes it without a phone call) and has found “the medical directors to be more than willing to work with the sleep center.”
Zachek’s success with patients, payors, and The Graves Gilbert Clinic showcases what HST can accomplish. By using home testing to reach more patients, and making staffing and other related changes accordingly, sleep centers can continue to keep their doors open—and even thrive.
Sree Roy is editor of Sleep Review.






Great article. Thanks for representing KY in the media.
May we post this on our website?
Thanks for the compliment and also for referring Dr. Zachek to us several years ago as an HST expert. To protect our copyrights, we can’t allow the full article to be posted on any other sites, but you are more than welcome to pull an excerpt from it onto your site and then link back here for your audience to read the full article.
Great article. Would like to see the nine page questionaire that Dr. Zachek gives to his patients.