Physician pay for existing patient visits tumbled dramatically last year, dropping by as much as a third as payors continued to reduce costs by cutting pay for services, and began experimenting with “value-based” pay models, according to the results of the Fee Schedule Survey by Physicians Practice, America’s Leading Business Journal for Physicians.
Pay rates to doctors have declined or remained flat in virtually every year since Physicians Practice began its annual survey in 2001. But last year’s cuts were particularly steep, especially on services to existing patients, said Bob Keaveney, Physicians Practice‘s editorial director.
For example, average reimbursement for the lowest-complexity diagnostic code for an existing patient (code 99211) dropped by a third, from $30 in 2011 to $20 last year. A midlevel code 99213 dropped 27 percent to $49.
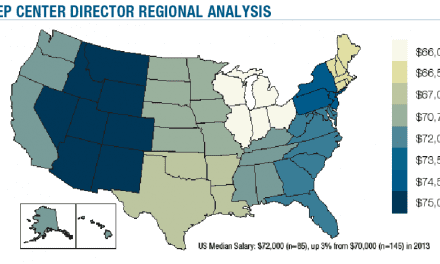
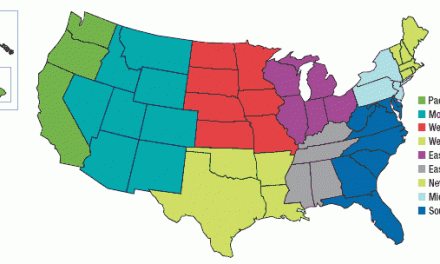
Physicians Practice surveys practices annually on what they are paid on average for common medical codes from all of their payors. The Physicians Practice Fee Schedule Survey, which in 2012 included more than 1,300 respondents from every part of the country, is the only broad-scale analysis of physicians’ reimbursement rates.
Pay for most new-patient visits increased modestly last year. The biggest increase was for the least-complex new-patient code, 99201, which rose 12 percent to $57.20. Smaller bumps were seen for the other new-patient codes, except the highest-complexity 99205, which declined slightly.
“Even the modest pay bumps are probably temporary,” Keaveney said. “I think 2013 is going to be another difficult year for physicians, as payors continue to try to control health costs by holding down reimbursement.”
The survey also found that the switch from a strictly fee-for-service pay model to one designed to pay for “value” has begun. One in five respondents said that some of their income last year came from non-fee-for-service contracts, and about one in four respondents anticipated more of the same this year.